What Is the Probability That Less Than 20 Preemies Are Born Out of the 250 Babies?
- Review
- Open up Admission
- Published:
Born Besides Soon: The global epidemiology of 15 million preterm births
Reproductive Health volume 10, Article number:S2 (2013) Cite this article
Abstract
This second paper in the Born As well Before long supplement presents a review of the epidemiology of preterm birth, and its burden globally, including priorities for activity to ameliorate the data. Worldwide an estimated 11.ane% of all livebirths in 2010 were born preterm (xiv.9 one thousand thousand babies born before 37 weeks of gestation), with preterm nativity rates increasing in most countries with reliable tendency data. Direct complications of preterm birth business relationship for ane 1000000 deaths each yr, and preterm nativity is a chance factor in over 50% of all neonatal deaths. In addition, preterm nativity tin can result in a range of long-term complications in survivors, with the frequency and severity of adverse outcomes rise with decreasing gestational age and decreasing quality of care. The economic costs of preterm birth are big in terms of firsthand neonatal intensive intendance, ongoing long-term complex wellness needs, as well as lost economical productivity. Preterm birth is a syndrome with a variety of causes and underlying factors usually divided into spontaneous and provider-initiated preterm births. Consistent recording of all pregnancy outcomes, including stillbirths, and standard application of preterm definitions is important in all settings to advance both the understanding and the monitoring of trends. Context specific innovative solutions to prevent preterm birth and hence reduce preterm nativity rates all around the world are urgently needed. Strengthened information systems are required to adequately track trends in preterm nativity rates and program effectiveness. These efforts must be coupled with action now to implement improved antenatal, obstetric and newborn intendance to increase survival and reduce disability among those born too shortly.
Declaration
This article is part of a supplement jointly funded by Save the Children's Saving Newborn Lives programme through a grant from The Bill & Melinda Gates Foundation and March of Dimes Foundation and published in collaboration with the Partnership for Maternal, Newborn and Child Health and the World Wellness System (WHO). The original article was published in PDF format in the WHO Report "Born Too Shortly: the global activeness study on preterm nascency" (ISBN 978 92 4 150343 30), which involved collaboration from more than 50 organizations. The article has been reformatted for periodical publication and has undergone peer review according to Reproductive Health'southward standard process for supplements and may characteristic some variations in content when compared to the original report. This co-publication makes the article bachelor to the community in a full-text format.
Why focus on preterm nativity?
Preterm birth is a major cause of death and a significant cause of long-term loss of human potential among survivors all around the world. Complications of preterm nascency are the unmarried largest directly cause of neonatal deaths, responsible for 35% of the world'south 3.1 million deaths a year, and the second most mutual cause of under-five deaths after pneumonia (Figure 1). In nigh all high- and middle-income countries of the earth, preterm birth is the leading cause of child death [1]. Being built-in preterm also increases a baby's risk of dying due to other causes, especially from neonatal infections [2] with preterm birth estimated to be a risk factor in at to the lowest degree l% of all neonatal deaths [3].
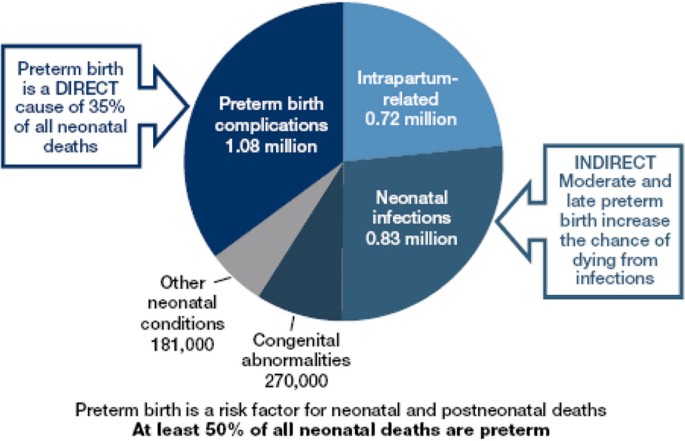
Estimated distribution of causes of iii.1 one thousand thousand neonatal deaths in 193 countries in 2010. Source: Updated from Lawn et al., 2005, using information from 2010 published in Liu Fifty, et al., 2012.
Addressing preterm nascency is essential for accelerating progress towards Millennium Development Goal 4 [4, five]. In addition to its significant contribution to mortality, the consequence of preterm birth amongst some survivors may go along throughout life, impairing neuro-developmental performance through increasing the risk of cerebral palsy, learning impairment and visual disorders and affecting long-term physical health with a higher risk of disease [6]. These effects exert a heavy burden on families, guild and the health system (Table 1) [7, eight]. Hence, preterm nativity is one the largest single conditions in the Global Burden of Disease analysis given the high mortality and the considerable hazard of lifelong impairment [9].
Information on preterm nascence rates are not routinely collected in many countries and, where bachelor, are frequently not reported using a standard international definition. Fourth dimension serial using consequent definitions are lacking for all but a few countries, making comparison within and between countries challenging. In high-income countries with reliable data, despite several decades of efforts, preterm birth rates appear to take increased from 1990 to 2010 [10–12], although the Usa reports a slight decrease in the rates of belatedly preterm birth (34 to <37 completed weeks) since 2007 [xiii].
Contempo estimates of preterm birth rates (all live births earlier 37 completed weeks) for 184 countries in 2010 and a time series for 65 countries with sufficient data suggest that fourteen.9 1000000 (dubiety range: 12.3-18.1 million) babies were born preterm in 2010 [14]. This paper reviews the epidemiology of preterm birth, and makes recommendations for efforts to improve the information and use the data for activity to accost preterm birth.
Agreement the information
Preterm birth -- what is information technology?
Defining preterm birth
Preterm nativity is defined by WHO equally all births before 37 completed weeks of gestation or fewer than 259 days since the first day of a woman's last menstrual period [15]. Preterm nascence can be farther sub-divided based on gestational age: extremely preterm (<28 weeks), very preterm (28 - <32 weeks) and moderate preterm (32 - <37 completed weeks of gestation) (Figure two). Moderate preterm birth may exist further split to focus on late pre-term nascency (34 - <37 completed weeks). The 37 week cut off is somewhat arbitrary, and information technology is now recognized that whilst the risks associated with preterm birth are greater the lower the gestational historic period, even babies born at 37 or 38 weeks accept higher risks than those born at 40 weeks gestation [xvi].
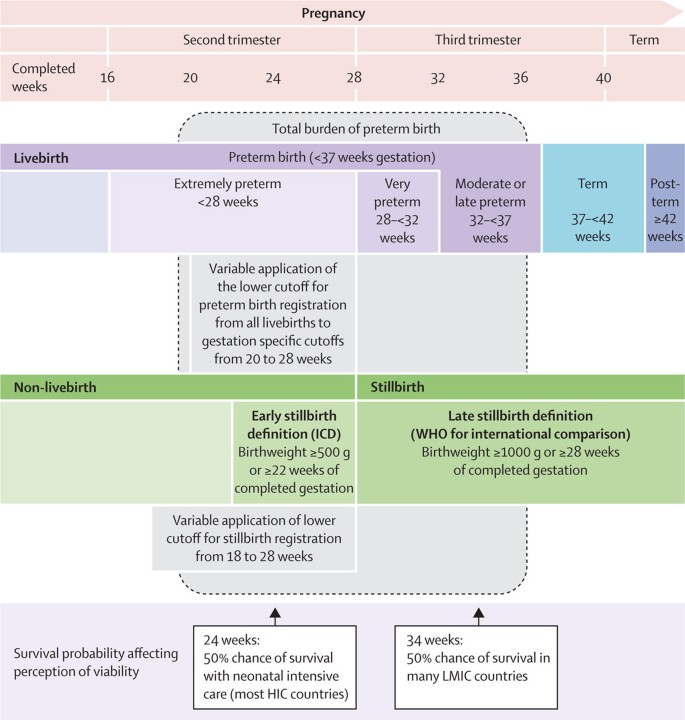
Overview of definitions for preterm birth and related pregnancy outcomes. Source: Reproduced with permission from Blencowe et al. (2012) National, regional and worldwide estimates of preterm birth rates in the year 2010 with fourth dimension trends since 1990 for selected countries: a systematic analysis and implications. Lancet 379(9832): 2162-2172.
The international definition for stillbirth charge per unit clearly states to utilize stillbirths > 1,000 chiliad or 28 weeks gestation, improving the ability to compare rates across countries and times [17, 18]. For preterm nascency, International Classification of Affliction (ICD) encourages the inclusion of all live births. This definition has no lower boundary, which complicates the comparison of reported rates both between countries and within countries over time since perceptions of viability of extremely preterm babies change with increasingly sophisticated neonatal intensive intendance, and some countries only include live births after a specific cut-off, for example, 22 weeks. In add-on, other reports utilize non-standard cutting-offs for upper gestational age (due east.g., including babies born at up to 38 completed weeks of gestation).
In many high-and middle-income countries, the official definitions of live birth or stillbirth have changed over time. Even without an explicit lower gestational historic period cut-off in national definitions, the medical care given and whether or not birth and death registration occurs may depend on these perceptions of viability [19, twenty]. Hence, even if no "official" lower gestational age cutting-off is specified for recording a live birth, misclassification of a livebirth to stillbirth is more mutual if the medical squad perceives the baby to be extremely preterm and thus less likely to survive [20]. Eighty percent of all stillbirths in high-income countries are born preterm, accounting for 5% of all preterm births. Counting only live births underestimates the true burden of preterm nascence [21, 22].
In addition to the definition and perceived viability issue, some reports include simply singleton live births, complicating comparison even farther. From a public health perspective and for the purposes of policy and planning, the total number of preterm births is the measure of interest.
Preterm nascency - why does it occur?
Preterm nascence is a syndrome with a variety of causes which tin can be classified into two broad subtypes: (1) spontaneous preterm nascence (spontaneous onset of labour or following prelabour premature rupture of membranes (pPROM)) and (2) provider-initiated preterm birth (defined as induction of labor or elective caesarean birth before 37 completed weeks of gestation for maternal or fetal indications (both "urgent" or "discretionary"), or other non-medical reasons) (Table 2) [23].
Spontaneous preterm birth is a multi-factorial process, resulting from the interplay of factors causing the uterus to change from quiescence to active contractions and to birth earlier 37 completed weeks of gestation. The precursors to spontaneous preterm nativity vary by gestational historic period [24], and social and environmental factors, but the cause of spontaneous preterm labor remains unidentified in up to one-half of all cases [25]. Maternal history of preterm birth is a potent adventure factor and most probable driven by the interaction of genetic, epigenetic and environmental risk factors [26]. Many maternal factors have been associated with an increased risk of spontaneous preterm birth, including young or advanced maternal age, curt inter-pregnancy intervals and low maternal body mass index [27, 28].
Another important risk cistron is uterine over distension with multiple pregnancy. Multiple pregnancies (twins, triplets, etc.) deport nearly 10 times the take chances of preterm birth compared to singleton births [29]. Naturally occurring multiple pregnancies vary amongst indigenous groups with reported rates from i in 40 in Westward Africa to 1 in 200 in Japan, just a large contributor to the incidence of multiple pregnancies has been rising maternal historic period and the increasing availability of assisted conception in high-income countries [30]. This has led to a large increment in the number of births of twins and triplets in many of these countries. For example, England and Wales, French republic and the United states reported fifty to threescore% increases in the twin charge per unit from the mid-1970s to 1998, with some countries (e.g. Republic of Korea) reporting even larger increases [31]. More recent policies, limiting the number of embryos transferred during in vitro fertilisation may accept begun to reverse this trend in some countries [32], while others keep to report increasing multiple birth rates [33, 34].
Infection plays an important office in preterm birth. Urinary tract infections, malaria, bacterial vaginosis, HIV and syphilis are all associated with increased risk of preterm nativity [35]. In addition, other weather condition have more than recently been shown to exist associated with infection, e.g., "cervical insufficiency" resulting from ascending intrauterine infection and inflammation with secondary premature cervical shortening [36].
Some lifestyle factors that contribute to spontaneous preterm birth include stress and excessive physical piece of work or long times spent standing [28]. Smoking and excessive alcohol consumption as well as periodontal disease likewise have been associated with increased gamble of preterm nascency [35].
Preterm nascence is both more common in boys, with around 55% of all preterm births occurring in males [37], and is associated with a higher risk of dying when compared to girls born at a like gestation [38]. The office of ethnicity in preterm nativity (other than through twinning rates) has been widely debated, but evidence supporting a variation in normal gestational length with ethnic group has been reported in many population-based studies since the 1970s [39]. While this variation has been linked to socioeconomic and lifestyle factors in some studies, recent studies propose a role for genetics. For example, babies of blackness African beginnings tend to be born before than Caucasian babies [24, 40]. However, for a given gestational age, babies of black African ancestry have less respiratory distress [41], lower neonatal mortality [42] and are less likely to require special care than Caucasian babies [24]. Babies with congenital abnormalities are more likely to exist born preterm, but are frequently excluded from studies reporting preterm nascence rates. Few national-level data on the prevalence of the run a risk factors for preterm birth are bachelor for modelling preterm birth rates.
The number and causes of provider-initiated preterm birth are more variable. Globally, the highest brunt countries have very low levels due to lower coverage of pregnancy monitoring and low caesarean nascency rates (less than five% in most African countries). However, in a recent written report in the United States, more than than half of all provider-initiated pre-term births at 34 to 36 weeks gestation were carried out in absenteeism of a strong medical indication [43]. Unintended preterm birth also can occur with the elective delivery of a baby thought to be term due to errors in gestational age assessment [44]. Clinical conditions underlying medically-indicated preterm nascence tin can exist divided into maternal and fetal of which severe preeclampsia, placental abruption, uterine rupture, cholestasis, fetal distress and fetal growth restriction with abnormal tests are some of the more important directly causes recognized [39]. Underlying maternal weather (due east.thou., renal disease, hypertension, obesity and diabetes) increase the risk of maternal complications (east.g., preeclampsia) and medically-indicated preterm nascence. The worldwide epidemic of obesity and diabetes is, thus, likely to become an increasingly important contributor to global preterm birth. In 1 region in the Britain, 17% of all babies born to diabetic mothers were preterm, more than double the rate in the general population [24]. Both maternal and fetal factors are more than oft seen in pregnancies occurring afterwards assisted fertility treatments, thus increasing the risk of both spontaneous and provider-initiated preterm births [44, 45].
Differentiating the causes of preterm nascency is particularly of import in countries where cesarean nascence is common. Virtually 40% of preterm births in France and the United states of america were reported to exist provider-initiated in 2000, compared to just over 20% in Scotland and the Netherlands. The levels of provider-initiated preterm births are increasing in all these countries in part due to more aggressive policies for caesarean section for poor foetal growth [46, 47]. In the United states, this increase is reported to exist at least in function responsible for the overall increase in the preterm nascence rate from 1990 to 2007 and the decline in perinatal mortality [39]. No population-based studies are available from low- or middle-income countries. However, of the babies built-in preterm in tertiary facilities in low- and middle-income countries, the reported proportion of preterm births that were provider-initiated ranged from effectually 20% in Sudan and Thailand to well-nigh 40% in 51 facilities in Latin America and a teaching infirmary in Ghana [48–51]. Even so, provider-initiated preterm births will represent a relatively smaller proportion of all preterm births in these countries where admission to diagnostic tools is limited. These pregnancies, if non delivered electively, volition follow their natural history, and may frequently end in spontaneous preterm birth (live or stillbirth)[52].
Preterm nascency--how is information technology measured?
There are many challenges to measuring preterm birth rates that have inhibited national data interpretation and multi-state assessment. In improver to the variable application of the definition, the varying methods used to measure gestational age and the differences in example ascertainment and registration complicate the interpretation of preterm birth rates across and within nations.
Assessing gestational age
Measurement of gestational age has changed over time. Equally the dominant issue of gestational historic period on survival and long-term damage has become apparent over the last 30 years, perinatal epidemiology has shifted from measuring birthweight solitary to focusing on gestational age. However, many studies, even of related pregnancy outcomes, keep to omit key measures of gestational historic period. The most authentic "gold standard" for cess is routine early on ultrasound assessment together with foetal measurements, ideally in the first trimester. Gestational assessment based on the date of last menstrual flow (LMP) was previously the virtually widespread method used and remains the only available method in many settings. It assumes that formulation occurs on the same solar day as ovulation (fourteen days afterwards the onset of the LMP). Information technology has depression accuracy due to considerable variation in length of menstrual cycle among women, conception occurring upwards to several days subsequently ovulation and the recall of the date of LMP being bailiwick to errors [53]. Many countries now use "best obstetric estimate," combining ultrasound and LMP as an approach to guess gestational age. The algorithm used tin accept a large bear on on the number of preterm births reported. For case, a big study from a Canadian education hospital found a preterm rate of 9.1% when assessed using ultrasound alone, compared to vii.eight% when using LMP and ultrasound [31].
Any method using ultrasound requires skilled technicians, equipment and for maximum accuracy, first-trimester antenatal clinic attendance. These are not common in low-income gear up tings where the majority of preterm births occur. Alternative approaches to LMP in these gear up tings include clinical assessment of the newborn after birth, fundal superlative or birthweight as a surrogate. While birthweight is closely linked with gestational historic period, it cannot exist used interchangeably since there is a range of "normal" birthweight for a given gestational age and gender. Birthweight is likely to overestimate preterm nascence rates in some settings, particularly in South asia where a high proportion of babies are small for gestational age.
Accounting for all births
The recording of births and deaths and the likelihood of agile medical intervention after preterm birth are affected by perceptions of viability and social and economic factors, especially in those built-in close to the lower gestational age cut-off used for registration. Any babe showing signs of beingness live at birth should be registered equally a livebirth regardless of the gestation [54]. The registration thresholds for stillbirths vary between countries from 16 to 28 weeks, and under-registration of both alive and stillbirths close to the registration boundary is well documented [55]. The cutting-off for viability has changed over time and varies beyond settings, with babies born at 22 to 24 weeks receiving full intensive care and surviving in some loftier-income countries, whilst babies born at upwardly to 32 weeks gestation are perceived as non-feasible in many low-resource settings. An case of this reporting bias is seen in high-income settings where the increase in numbers of extremely preterm (<28 weeks) births registered is likely to exist due to improved instance observation rather than a genuine increase in preterm births in this grouping [56] and three community cohorts from South Asia with high overall preterm birth rates of 14 to 20%, but low proportions (2%) of extremely preterm births (<28 weeks) compared to the proportion from pooled datasets from developed countries (5.three%). In addition, even where care is offered to these very preterm babies, intensive care may be rationed [57, 58].
Other cultural and social factors that take been reported to affect completeness of registration include provision of motherhood benefits for any birth subsequently the registration threshold, the demand to pay burial costs for a registered birth simply not for a miscarriage and increased hospital fees following a birth compared to a miscarriage [59]. In depression-income settings, a alive preterm birth may be counted every bit a stillbirth due to perceived non-viability or to "protect the mother" [55].
The definition of preterm nativity focuses on live-born babies only. Counting all preterm births, both live and stillborn, would be preferable to improve comparability especially given stillbirth/livebirth misclassification. An increasing proportion of all preterm infants born will exist stillborn with decreasing gestational historic period. The pathophysiology is like for live and stillbirths; thus, for the truthful public health burden, it is essential to count both preterm babies born alive and all stillbirths [23]. Until these nomenclature differences based on method (Tabular array iii), lower gestational historic period cut-offs for registration of preterm birth, the use of singleton versus all births (including multiples), the inclusion of live births versus total births (including live and stillbirths) and instance observation have been resolved, caution needs to be applied when interpreting regional and temporal variations in preterm birth rates.
Using the data for action
Preterm birth rates--where, and when?
Global, regional and national variation of preterm birth for the year 2010
New WHO estimates of global rates of preterm births indicate that of the 135 million alive births worldwide in 2010, xiv.nine million babies were built-in preterm, representing a preterm birth rate of 11.one% [14]. Over threescore% of preterm births occurred in sub-Saharan Africa and Southern asia where nine.i million births (12.8%) annually are estimated to be preterm (Figure 3). The high accented number of preterm births in Africa and Asia are related, in part, to high fertility and the large number of births in those two regions in comparison to other parts of the world.
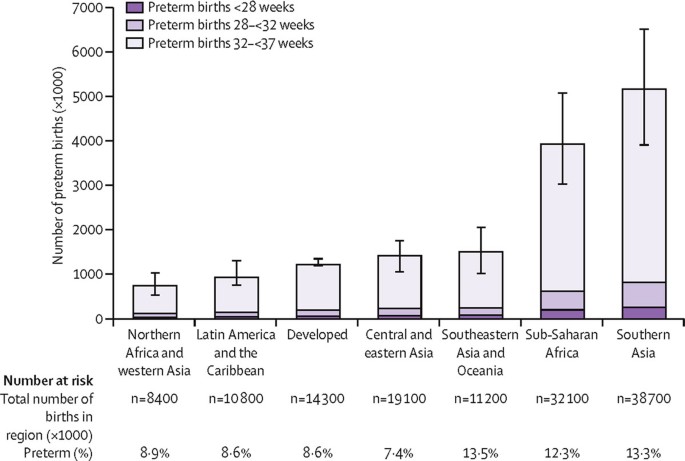
Preterm births past gestational age and region for the twelvemonth 2010. Based on Millennium Development Goal regions. Source: Reproduced with permission from Blencowe et al. (2012) National, regional and worldwide estimates of preterm nascency rates in the year 2010 with time trends since 1990 for selected countries: a systematic analysis and implications. Lancet 379(9832): 2162-2172.
The variation in the rate of preterm birth amidst regions and countries is substantial and yield a different picture to other conditions in that some high-income countries accept very loftier rates. Rates are highest on average for low-income countries (xi.8%), followed by lower middle-income countries (11.iii%) and lowest for upper centre- and high-income countries (nine.4% and 9.3%). Withal, relatively high preterm nascency rates are seen in many individual high-income countries where they contribute essentially to neonatal bloodshed and morbidity. Of the one.2 1000000 preterm births estimated to occur in high-income regions, more 0.five million (42%) occur in the United states. The highest rates by Millennium Evolution Goal Regions [60] are found in Southeastern and S Asia where xiii.4% of all live births are estimated to be preterm (Figure 3).
The uncertainty ranges in Effigy 3 are indicative of another trouble -- the huge data gaps for many regions of the world. Although these data gaps are specially great for Africa and Asia, in that location also are gaps in information from high-income countries. While information on preterm birth-associated mortality are lacking in these settings, worldwide at that place are almost no data currently on acute morbidities or long-term damage associated with prematurity, thus preventing even the most basic assessments of service needs.
The maps in Figure four describe preterm birth rates and the accented numbers of preterm nascency in 2010 by country. Estimated rates vary from around 5 in several Northern European countries to xviii.ane% in Malawi. The estimated preterm nascence rate is less than 10% in 88 countries, whilst 11 countries have estimated rates of 15% or more (Figure iv). The 10 countries with the highest numbers of estimated preterm births are Bharat, China, Nigeria, Islamic republic of pakistan, Indonesia, Usa, Bangladesh, the Philippines, Democratic Congo-brazzaville and Brazil (Figure 4). These ten countries account for 60% of all preterm births worldwide.
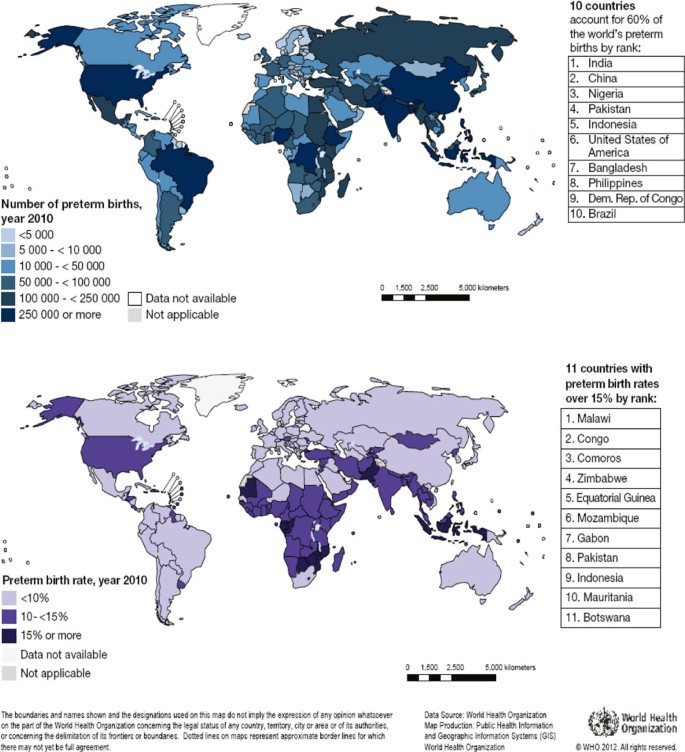
Preterm births in 2010. Source: Blencowe, H., et al. (2012) Affiliate 2: 15 million preterm births: Priorities for action based on national, regional and global estimates. In Born Too Soon: the Global Activeness Written report on Preterm Nativity. http://www.who.int/pmnch/media/news/2012/borntoosoon_chapter2.pdf 2012 [79]. Non applicable = not WHO Members State.
Mortality rates increase with decreasing gestational age, and babies who are both preterm and small for gestational age are at even higher risk [61]. Babies built-in at less than 32 weeks represent nearly 16% of all preterm births [14]. Across all regions, mortality and morbidity are highest among those babies although improvements in medical intendance have led to improved survival and long-term outcomes amidst very and extremely preterm babies in high-income countries [62]. In 1990, around 60% of babies born at less than 28 weeks gestation survived in high-income settings, with approximately ii-thirds surviving without impairment [63]. In these high-income countries, almost 95% of those born at 28 to 32 weeks survive, with more xc% surviving without impairment. In dissimilarity, in many low-income countries, merely thirty% of those born at 28 to 32 weeks survive, with almost all those born at <28 weeks dying in the first few days of life. In all settings, these very or extremely preterm babies account for the bulk of deaths, especially in low-income countries where even simple care is lacking [64].
Preterm births time trends 1990 to 2010
Absolute numbers and rates of preterm birth for 65 countries in Europe, the Americas and Australasia from 1990 to 2010 for these countries suggest an increasing burden of preterm birth [v]. This increase is partly explained past an increase in preterm births occurring at 32 to <37 weeks (tardily and moderate preterm) reported over the by decades in some countries [65]. Despite a reduction in the number of live births, the estimated number of preterm births in these countries increased from 2.0 million in 1990 to nearly 2.2 1000000 in 2010 [14]. Preterm nascency rate trends for low- and heart-income countries suggest an increase in some countries (east.g., China) and some regions (e.g., Southern asia) just given changes in the data type and the measurement of gestational age, these remain uncertain.
Priority policy and program deportment based on the information
In 2010, approximately xv one thousand thousand babies were born preterm, and more than one million died due to complications in the first month of life, more from indirect furnishings, and millions have a lifetime of impairment. The burden of preterm nascence is highest in low-income countries, particularly those in South asia. Yet unlike many other global health bug, preterm birth is truly a global trouble with a high burden being found in loftier-income countries as well (e.thou. the United States where virtually 1 in 8 babies is preterm). However, while the run a risk of preterm birth is high for both the poorest and the richest countries, in that location exists a major survival gap in some regions for babies who are preterm. In high-income settings, half of babies born at 24 weeks may survive, just in depression-income settings half of babies born at 32 weeks nonetheless dice due to a lack of basic care [64].
Preterm birth rates announced to be increasing in almost of the countries where data are available. Some of this increase may be accounted for by improved registration of the well-nigh preterm babies associated with increased viability and past improved gestational assessment, with change to well-nigh universal ultrasound for dating pregnancies in these settings. It may, nevertheless, represent a truthful increment. Possible reasons for this include increases in maternal age, access to infertility treatment, multiple pregnancies and underlying health bug in the mother, especially with increasing age of pregnancy and changes in obstetric practices with an increase in provider-initiated preterm births in moderate and late preterm infants who would not have otherwise been born preterm [46]. In the 1980s and 1990s, the increases seen in many high-income countries were attributed to higher multiple gestation and preterm birth rates amid assisted conceptions after treatment for sub-fertility. Recent changes in policies limiting the number of embryos that can be implanted take led to a reduction in preterm births due to assisted fertility treatments in many countries [63]. Even so, in many center-income regions with newer, relatively unregulated assisted fertility services, a similar increment may be seen if policies to annul this are not introduced and adhered to. A reduction in preterm nativity was reported from the 1960s to 1980s in a few countries (due east.g. Republic of finland, France, Scotland), and this was attributed, in part, to improved socioeconomic factors and antenatal care. For the majority of countries in low- and middle-income regions, it is not possible to estimate trends in preterm birth over fourth dimension as in that location are not sufficient data to provide reliable evidence of a time tendency for preterm nativity overall. Some countries in some regions (e.g. South and Eastern Asia) accept data suggesting possible increases in preterm nascence rates over fourth dimension, but this may stand for measurement artifact due to increases in data and data reliability.
Distinguishing spontaneous and provider-initiated preterm nascence is of importance to programs aiming to reduce preterm birth. For spontaneous preterm births, the underlying causes need to be understood and addressed while in the instance of provider-initiated preterm births both the underlying conditions (e.grand. preeclampsia) and obstetric policies and practices require assessment and to be addressed [66, 67].
The proportion of neonatal deaths attributed to preterm births is inversely related to neonatal mortality rates, because in countries with very high neonatal bloodshed, more deaths occur due to infections such every bit sepsis, pneumonia, diarrhea and tetanus as well every bit to intrapartum-related "birth asphyxia" [two]. However, although the proportion of deaths due to preterm nascence is lower in low-income countries than in high-income countries, the crusade-specific rates are much higher in low- and middle-income than in high-income countries. For example, in Afghanistan and Somalia, the estimated cause-specific rate for neonatal deaths directly due to preterm birth is xvi per 1,000 compared to Japan, Norway and Sweden where it is under 0.5 per i,000. This is due to the lack of even simple care for premature babies resulting in a major survival gap for babies depending on where they are built-in [64].
Preterm birth can consequence in a range of long-term complications in survivors, with the frequency and severity of adverse outcomes ascent with decreasing gestational age and decreasing quality of care (Table 1). Virtually babies born at less than 28 weeks need neonatal intensive intendance services to survive, and about babies 28 to 32 weeks volition demand special newborn care at a minimum. The availability and quality of these services are not however well established in many low- and middle-income countries. Many middle-income countries, currently scaling upwards neonatal intensive care, are only start to experience these long-term consequences in survivors. 43% of the estimated 0.9 1000000 preterm babies surviving with neurodevelopmental damage are from middle income countries [8]. These effects are near marked amongst survivors born extremely preterm; however, there is increasing show that all premature babies regardless of gestational age are at increased risk. The vast bulk (84%) of all preterm births occur at 32 to 36 weeks. Nigh of these infants will survive with adequate supportive care and without needing neonatal intensive care. However, even babies built-in at 34 to 36 weeks have been shown to have an increased risk of neonatal and baby death when compared with those born at term and contribute importantly to overall infant deaths [68]. Babies born at 34 to 36 weeks as well experience increased rates of short-term morbidity associated with prematurity (e.g., respiratory distress and intraventricular hemorrhage) than their peers built-in at term [69–71]. In the longer term, they have worse neurodevelopmental and school performance outcomes and increased take chances of cerebral palsy [72, 73]. On a global level, given their relatively larger numbers, babies born at 34 to 36 weeks are likely to have the greatest public health bear upon and to exist of the most importance in the planning of services (e.thou., training community health workers in Kangaroo Mother Intendance (KMC), essential newborn care and special intendance of the moderately preterm baby) [64].
We have highlighted the differences in preterm birth rates among countries, but marked disparities are likewise present within countries. For example, in the United States in 2009, reported preterm nascency rates were every bit loftier as 17.five% in black Americans, compared to but x.nine% in white Americans, with rates varying from around xi to 12% in those 20 to 35 years of age to more than than xv% in those under age 17 or over 40 [xiii]. Disparities inside countries need to be ameliorate understood in lodge to place high-chance groups and improve care.
The economic costs of preterm nascency are big in terms of the firsthand neonatal intensive care and ongoing long-term complex health needs often experienced. These costs, in add-on, are likely to rise as premature babies increasingly survive at earlier gestational ages in all regions. This survival as well volition result in the increased need for special education services and associated costs that volition identify an additional burden on afflicted families and the communities in which they live [74]. An increased awareness of the long-term consequences of preterm nascence (at all gestational ages) is required to fashion policies to back up these survivors and their families as office of a more generalised improvement in quality of intendance for those with disabilities in any given country. In many middle-income countries, preterm birth is an important cause of disability. For example, a third of all children under ten in schools for the visually impaired in Vietnam and more than than 40% of nether-5's in similar schools in Mexico accept incomprehension secondary to retinopathy of prematurity [75, 76].
Actions to improve the information
The estimates from the Built-in As well Before long report correspond a major step forward in terms of presenting the starting time-e'er national preterm birth estimates [77]. All the same, activity is required to improve the availability and quality of data from many countries and regions and, where information are beingness collected and analysed, to improve consistency among countries. These are vital side by side steps to monitor the progress of policies and programs aimed at reducing the large toll of preterm birth (Tabular array 4). Efforts in every state should be directed to increasing the coverage and systematic recording of all preterm births in a standard reporting format. Standardisation of the definition in terms of both the numerator (the number of preterm births) and the denominator (the number of all births) is essential if trends and rankings are to be truly comparable. Collecting data on both live and stillbirths separately will let farther quantification of the true burden, while data focusing on live births only are required for monitoring of neonatal and longer-term outcomes. These estimates indicate the large burden amongst live-born babies. However, in developed countries with available data, betwixt 5 and 10% of all preterm births are stillbirths, and the figure may exist higher in countries with lower levels of medicallyinduced preterm birth. Distinguishing between alive births and stillbirths may vary depending on local policies, the availability of intensive intendance and perceived viability of babies who are extremely preterm. If estimates for live-born preterm babies were linked to estimates for stillbirths, this would better tracking among countries and over time. Achieving consensus effectually the different types of preterm nascence and comparable case definitions, whilst challenging, are required where resources allow to further understand the complex syndrome of preterm nascence [23].
In many low- and center-income countries without wide-scale vital registration, no nationally representative data are bachelor on rates of preterm birth. Substantial investment and attention are required to improve vital registration systems and to account for all birth outcomes [78]. In the meantime, the amount of population-based information available in high-brunt countries could be dramatically increased to better inform hereafter estimates and monitor time trends if data on preterm birth rates were able to be included in nationally representative surveys such as the Demographic and Wellness Surveys (DHS), but this will require developing, testing and preparation in the use of preterm-specific survey-based tools which are not currently bachelor. The appearance of inexpensive portable ultrasound machines makes inclusion of routine early ultrasound scans in demographic surveillance sites or representative cohorts a promising route to increase data availability in these settings in the brusque term. Innovation for simpler, low-cost, sensitive and specific tools for assessing gestational age could meliorate both the coverage and quality of gestational age assessment. Information from hospital-based information systems would likewise be helpful, just potential option and other biases must exist taken into account. Simpler standardized tools to assess acute and long-term morbidities-associated preterm birth also are critically of import to inform program quality improvement to reduce the proportion of survivors with preventable damage.
Conclusion
There are sufficient data to justify activity now to reduce this big brunt of 15 million preterm births and more than than one million neonatal deaths. Innovative solutions to forestall preterm birth and hence reduce preterm birth rates all around the globe are urgently needed. This likewise requires strengthened information systems to adequately track trends in preterm birth rates and programme effectiveness. These efforts must be coupled with action now to implement improved antenatal, obstetric and newborn care to increase survival and reduce disability amidst those born as well soon. These are reviewed further in the following papers in this supplement.
Funding
HB and SC were funded through a grant from the Bill & Melinda Gates Foundation through the Child Health Epidemiology Reference Group. JL and MK were funded past the Bill & Melinda Gates Foundation though Save the Children's Saving Newborn Lives program.
Abbreviations
- pPROM:
-
prelabour premature rupture of membranes
- WHO:
-
World Health Organization.
References
-
Liu L, Johnson H, Cousens S, Perin J, Scott S, Lawn J, Ruden I, Campbell H, Cibulskis R, Mengying L: Global, regional and national causes of child bloodshed: an updated systematic analysis for 2010 with time trends since 2000. The Lancet. 2012, 379: 2151-2161. x.1016/S0140-6736(12)60560-1.
-
Lawn JE, Cousens S, Zupan J: iv one thousand thousand neonatal deaths: when? Where? Why?. Lancet. 2005, 365: 891-900. 10.1016/S0140-6736(05)71048-5.
-
Lawn JE, Kerber K, Enweronu-Laryea C, Cousens S: three.six million neonatal deaths - what is progressing and what is not?. Semin Perinatol. 2010, 34: 371-386. 10.1053/j.semperi.2010.09.011.
-
Millennium Development Goals Indicators. [http://mdgs.un.org/unsd/mdg/Default.aspx]
-
Howson CP, Kimmey MV, McDougall 50, Backyard JE: Born Too Soon: Preterm nativity matters. Reprod Health. 2013, x (Suppl 1): S1-10.1186/1742-4755-10-S1-S1.
-
Rogers LK, Velten M: Maternal inflammation, growth retardation, and preterm nativity: insights into developed cardiovascular disease. Life Sci. 2011, 89: 417-421. 10.1016/j.lfs.2011.07.017.
-
Preterm Birth: Causes, Consequences, and Prevention. [http://www.iom.edu/Reports/2006/Preterm-Nativity-Causes-Consequences-and-Prevention.aspx]
-
Blencowe H, Lee Air conditioning, Cousens S, Bahalim A, Narwal R, Zhong Due north, Chou D, Say L, Modi N, Katz J: Preterm birth associated neurodevelopmental impairment estimates at regional and global level for 2010. Pediatric Research. 2013
-
Murray CJ, Vos T, Lozano R, Naghavi M, Flaxman AD, Michaud C, Ezzati M, Shibuya Chiliad, Salomon JA, Abdalla Due south: Disability-adjusted life years (DALYs) for 291 diseases and injuries in 21 regions, 1990-2010: a systematic analysis for the Global Burden of Disease Study 2010. Lancet. 2012, 380: 2197-2223. ten.1016/S0140-6736(12)61689-4.
-
Langhoff-Roos J, Kesmodel U, Jacobsson B, Rasmussen Southward, Vogel I: Spontaneous preterm delivery in primiparous women at depression risk in Denmark: population based study. BMJ. 2006, 332: 937-939. ten.1136/bmj.38751.524132.2F.
-
Martin JA, Hamilton Be, Sutton PD, Ventura SJ, Mathews TJ, Kirmeyer S, Osterman MJ: Births: terminal data for 2007. Natl Vital Stat Rep. 2010, 58: ane-85.
-
Thompson JM, Irgens LM, Rasmussen S, Daltveit AK: Secular trends in socioeconomic status and the implications for preterm birth. Paediatr Perinat Epidemiol. 2006, 20: 182-187. x.1111/j.1365-3016.2006.00711.x.
-
Hamilton Exist, Ventura P, Osterman M, Kirmeyer S, Mathews MS, Wilson Eastward: Births: Final Information for 2009. National Vital Staistic Reports. 2011, lx:
-
Blencowe H, Cousens S, Oestergaard MZ, Chou D, Moller AB, Narwal R, Adler A, Vera Garcia C, Rohde S, Say L, Lawn JE: National, regional, and worldwide estimates of preterm birth rates in the yr 2010 with time trends since 1990 for selected countries: a systematic analysis and implications. Lancet. 2012, 379: 2162-2172. 10.1016/S0140-6736(12)60820-four.
-
WHO: WHO: recommended definitions, terminology and format for statistical tables related to the perinatal menstruum and utilize of a new document for crusade of perinatal deaths. Modifications recommended by FIGO as amended Oct 14, 1976. Acta Obstet Gynecol Scand. 1977, 56: 247-253.
-
Marlow Due north: Full term; an artificial concept. Arch Dis Kid Fetal Neonatal Ed. 2012, 97: F158-10.1136/fetalneonatal-2011-301507.
-
Lawn JE, Blencowe H, Pattinson R, Cousens S, Kumar R, Ibiebele I, Gardosi J, Twenty-four hours LT, Stanton C: Stillbirths: Where? When? Why? How to make the information count?. Lancet. 2011, 377: 1448-1463. x.1016/S0140-6736(10)62187-three.
-
Cousens Due south, Blencowe H, Stanton C, Chou D, Ahmed South, Steinhardt L, Creanga AA, Tuncalp O, Balsara ZP, Gupta South: National, regional, and worldwide estimates of stillbirth rates in 2009 with trends since 1995: a systematic analysis. Lancet. 2011, 377: 1319-1330. x.1016/S0140-6736(10)62310-0.
-
Goldenberg RL, Nelson KG, Dyer RL, Wayne J: The variability of viability: the effect of physicians' perceptions of viability on the survival of very lowbirth weight infants. Am J Obstet Gynecol. 1982, 143: 678-684.
-
Sanders MR, Donohue PK, Oberdorf MA, Rosenkrantz TS, Allen MC: Touch on of the perception of viability on resource allocation in the neonatal intensive care unit. J Perinatol. 1998, eighteen: 347-351.
-
Flenady V, Middleton P, Smith GC, Duke W, Erwich JJ, Khong TY, Neilson J, Ezzati Yard, Koopmans L, Ellwood D: Stillbirths: the way forrad in highincome countries. Lancet. 2011, 377: 1703-1717. 10.1016/S0140-6736(eleven)60064-0.
-
Kramer MS, Papageorghiou A, Culhane J, Bhutta Z, Goldenberg RL, Gravett M, Iams JD, Conde-Agudelo A, Waller Southward, Barros F: Challenges in defining and classifying the preterm birth syndrome. Am J Obstet Gynecol. 2012, 206: 108-112. ten.1016/j.ajog.2011.10.864.
-
Goldenberg RL, Gravett MG, Iams J, Papageorghiou AT, Waller SA, Kramer Chiliad, Culhane J, Barros F, Conde-Agudelo A, Bhutta ZA: The preterm nascency syndrome: issues to consider in creating a classification system. Am J Obstet Gynecol. 2012, 206: 113-118. 10.1016/j.ajog.2011.10.865.
-
Steer P: The epidemiology of preterm labour. BJOG. 2005, 112 (Suppl one): 1-3.
-
Menon R: Spontaneous preterm birth, a clinical dilemma: etiologic, pathophysiologic and genetic heterogeneities and racial disparity. Acta Obstet Gynecol Scand. 2008, 87: 590-600. 10.1080/00016340802005126.
-
Plunkett J, Muglia LJ: Genetic contributions to preterm birth: implications from epidemiological and genetic association studies. Ann Med. 2008, 40: 167-195. 10.1080/07853890701806181.
-
Goldenberg RL, Culhane JF, Iams JD, Romero R: Epidemiology and causes of preterm nascence. Lancet. 2008, 371: 75-84. x.1016/S0140-6736(08)60074-4.
-
Muglia LJ, Katz M: The enigma of spontaneous preterm birth. N Engl J Med. 2010, 362: 529-535. 10.1056/NEJMra0904308.
-
Blondel B, Macfarlane A, Gissler M, Breart One thousand, Zeitlin J: Preterm birth and multiple pregnancy in European countries participating in the PERISTAT projection. BJOG. 2006, 113: 528-535. 10.1111/j.1471-0528.2006.00923.x.
-
Felberbaum RE: Multiple pregnancies after assisted reproduction - international comparison. Reprod Biomed Online. 2007, 53-60. xv Suppl three
-
Blondel B, Kaminski M: Trends in the occurrence, determinants, and consequences of multiple births. Semin Perinatol. 2002, 26: 239-249. 10.1053/sper.2002.34775.
-
Kaprio J MR: Demographic trends in Nordic countries. Multiple Pregnancy: Epidemiology, Gestation & Perinatal Weather condition 2nd edn. Edited by: Blickstein I KL. 2005, London: Taylor & Francis, 22-25. two
-
Lim JW: The changing trends in live nascence statistics in Korea, 1970 to 2010. Korean J Pediatr. 2011, 54: 429-435. x.3345/kjp.2011.54.11.429.
-
Hamilton Exist, Sutton PD, Ventura SJ, Mathews TJ, Osterman MJ: Births: final data for 2008. Natl Vital Stat Rep. 2010, 59: 1, 3-71.
-
Gravett MG, Rubens CE, Nunes TM: Global study on preterm nascency and stillbirth (2 of 7): discovery science. BMC Pregnancy Childbirth. 2010, S2-10 Suppl ane
-
Lee SE, Romero R, Park CW, Jun JK, Yoon BH: The frequency and significance of intraamniotic inflammation in patients with cervical insuffi ciency. Am J Obstet Gynecol. 2008, 198: 633 e631-638.
-
Zeitlin J, Saurel-Cubizolles MJ, De Mouzon J, Rivera 50, Ancel PY, Blondel B, Kaminski M: Fetal sex and preterm birth: are males at greater take a chance?. Hum Reprod. 2002, 17: 2762-2768. 10.1093/humrep/17.ten.2762.
-
Kent AL, Wright IM, Abdel-Latif ME: Mortality and agin neurologic outcomes are greater in preterm male infants. Pediatrics. 2012, 129: 124-131. ten.1542/peds.2011-1578.
-
Ananth CV, Vintzileos AM: Epidemiology of preterm nascence and its clinical subtypes. J Matern Fetal Neonatal Med. 2006, nineteen: 773-782. 10.1080/14767050600965882.
-
Patel RR, Steer P, Doyle P, Little MP, Elliott P: Does gestation vary by ethnic group? A London-based study of over 122,000 pregnancies with spontaneous onset of labour. Int J Epidemiol. 2004, 33: 107-113. 10.1093/ije/dyg238.
-
Farrell PM, Forest RE: Epidemiology of hyaline membrane disease in the Us: analysis of national mortality statistics. Pediatrics. 1976, 58: 167-176.
-
Alexander GR, Kogan One thousand, Bader D, Carlo W, Allen M, Mor J: US nascency weight/ gestational age-specific neonatal mortality: 1995-1997 rates for whites, hispanics, and blacks. Pediatrics. 2003, 111: e61-66. 10.1542/peds.111.1.e61.
-
Gyamfi-Bannerman C, Fuchs KM, Immature OM, Hoff man MK: Nonspontaneous late preterm nativity: etiology and outcomes. Am J Obstet Gynecol. 2011, 205: 456 e451-456.
-
Mukhopadhaya Northward, Arulkumaran S: Reproductive outcomes after in-vitro fertilization. Curr Opin Obstet Gynecol. 2007, 19: 113-119. 10.1097/GCO.0b013e32807fb199.
-
Kalra SK, Molinaro TA: The association of in vitro fertilization and perinatal morbidity. Semin Reprod Med. 2008, 26: 423-435. x.1055/southward-0028-1087108.
-
Joseph KS, Demissie Thou, Kramer MS: Obstetric intervention, stillbirth, and preterm birth. Semin Perinatol. 2002, 26: 250-259. x.1053/sper.2002.34769.
-
Joseph KS, Kramer MS, Marcoux S, Ohlsson A, Wen SW, Allen A, Platt R: Determinants of preterm birth rates in Canada from 1981 through 1983 and from 1992 through 1994. N Engl J Med. 1998, 339: 1434-1439. 10.1056/NEJM199811123392004.
-
Barros FC, Velez Mdel P: Temporal trends of preterm nascency subtypes and neonatal outcomes. Obstet Gynecol. 2006, 107: 1035-1041. x.1097/01.AOG.0000215984.36989.5e.
-
Alhaj AM, Radi EA, Adam I: Epidemiology of preterm nativity in Omdurman Maternity hospital, Sudan. J Matern Fetal Neonatal Med. 2010, 23: 131-134. ten.3109/14767050903067345.
-
Ip M, Peyman Due east, Lohsoonthorn 5, Williams MA: A case-command study of preterm commitment chance factors according to clinical subtypes and severity. J Obstet Gynaecol Res. 2010, 36: 34-44. 10.1111/j.1447-0756.2009.01087.x.
-
Nkyekyer Thou, Enweronu-Laryea C, Boafor T: Singleton preterm births in korle bu teaching infirmary, accra, ghana-origins and outcomes. Ghana Med J. 2006, 40: 93-98.
-
Klebanoff MA, Shiono PH: Top down, lesser up and inside out: reflections on preterm nativity. Paediatr Perinat Epidemiol. 1995, 9: 125-129. 10.1111/j.1365-3016.1995.tb00126.x.
-
Kramer MS, McLean FH, Boyd ME, Usher RH: The validity of gestational historic period estimation by menstrual dating in term, preterm, and postterm gestations. JAMA. 1988, 260: 3306-3308. ten.1001/jama.1988.03410220090034.
-
ICD-10: international statistical classificiation of diseases and related wellness problems: tenth revision. 2nd ed. [http://world wide web.who.int/classifications/icd/ICD-10_2nd_ed_volume2.pdf]
-
Froen JF, Gordijn SJ, Abdel-Aleem H, Bergsjo P, Betran A, Duke CW, Fauveau V, Flenady V, Hinderaker SG, Hofmeyr GJ: Making stillbirths count, making numbers talk-bug in information collection for stillbirths. BMC Pregnancy Childbirth. 2009, ix: 58-10.1186/1471-2393-nine-58.
-
Annual Reports for the years 1991 and 1999. Melbourne:Consultative Council on Obstetrics and Paediatric Bloodshed and Morbidity, 1992 and 2001.
-
MRC PPIP Users, the Saving Babies Technical Task Team: Saving Babies 2008-2009. 2010, 7th report on perinatal intendance in South Africa
-
Miljeteig I, Johansson KA, Sayeed SA, Norheim OF: Cease-of-life decisions as bedside rationing. An ethical analysis of life support restrictions in an Indian neonatal unit. J Med Ethics. 2010, 36: 473-478. ten.1136/jme.2010.035535.
-
Lumley J: Defining the problem: the epidemiology of preterm nascence. BJOG. 2003, 110 (Suppl xx): 3-7.
-
Millennium, Development Goals Indicators. 2012, Accessed tertiary January, [http://mdgs.un.org/unsd/mdg/Default.aspx]
-
Katz J, Lee AC, Kozuki N, Backyard JE, Cousens S, Blencowe H, Ezzati M, Bhutta ZA, Marchant T, Willey BA: Mortality risk in preterm and small-for-gestational-age infants in depression-income and centre-income countries: a pooled country assay. Lancet. 2013
-
Saigal South, Doyle LW: An overview of mortality and sequelae of preterm nascence from infancy to adulthood. Lancet. 2008, 371: 261-269. 10.1016/S0140-6736(08)60136-1.
-
Mohangoo Advertisement, Buitendijk SE, Szamotulska K, Chalmers J, Irgens LM, Bolumar F, Nijhuis JG, Zeitlin J: Gestational age patterns of fetal and neonatal bloodshed in europe: results from the Euro-Peristat project. PLoS One. 2011, 6: e24727-10.1371/journal.pone.0024727.
-
Backyard JE, Davidge R, Paul VK, von Xylander S, de Graft Johnson J, Costello A, Kinney MV, Segre J, Molyneux L: Born Too Presently: Care for the preterm baby. Reprod Wellness. 2013, 10 (Suppl one): S5-10.1186/1742-4755-10-S1-S5.
-
Davidoff MJ, Dias T, Damus K, Russell R, Bettegowda VR, Dolan S, Schwarz RH, Dark-green NS, Petrini J: Changes in the gestational historic period distribution among U.S. singleton births: impact on rates of late preterm birth, 1992 to 2002. Semin Perinatol. 2006, thirty: 8-15. 10.1053/j.semperi.2006.01.009.
-
Dean SV, Mason EM, Howson CP, Lassi ZS, Imam AM, Bhutta ZA: Born Too Shortly: Care before and between pregnancy to prevent preterm births: from evidence to activity. Reprod Health. 2013, 10 (Suppl 1): S3-x.1186/1742-4755-ten-S1-S3.
-
Requejo J, Althabe F, Merialdi 1000, Keller K, Katz J, Menon R: Born Too Shortly: Care during pregnancy and childbirth to reduce preterm deliveries and improve health outcomes of the preterm infant. Reprod Health. 2013, 10 (Suppl 1): S4-ten.1186/1742-4755-ten-S1-S4.
-
Kramer MS, Demissie 1000, Yang H, Platt RW, Sauve R, Liston R: The contribution of balmy and moderate preterm nascence to infant mortality. Fetal and Infant Health Study Grouping of the Canadian Perinatal Surveillance System. JAMA. 2000, 284: 843-849. x.1001/jama.284.7.843.
-
Femitha P, Bhat BV: Early Neonatal Outcome in Late Preterms. Indian J Pediatr. 2011
-
Escobar GJ, Clark RH, Greene JD: Short-term outcomes of infants built-in at 35 and 36 weeks gestation: nosotros need to ask more questions. Semin Perinatol. 2006, thirty: 28-33. x.1053/j.semperi.2006.01.005.
-
Teune MJ, Bakhuizen S, Gyamfi Bannerman C, Opmeer BC, van Kaam AH, van Wassenaer AG, Morris JM, Mol BW: A systematic review of severe morbidity in infants born late preterm. Am J Obstet Gynecol. 2011, 205: 374 e371-379.
-
Quigley MA, Poulsen G, Boyle Due east, Wolke D, Field D, Alfi revic Z, Kurinczuk JJ: Early on term and belatedly preterm birth are associated with poorer schoolhouse performance at age five years: a cohort study. Arch Dis Child Fetal Neonatal Ed. 2012
-
Woythaler MA, McCormick MC, Smith VC: Late preterm infants have worse 24-calendar month neurodevelopmental outcomes than term infants. Pediatrics. 2011, 127: e622-629. 10.1542/peds.2009-3598.
-
Petrou S, Eddama O, Mangham 50: A structured review of the contempo literature on the economic consequences of preterm birth. Arch Dis Kid Fetal Neonatal Ed. 2011, 96: F225-232. 10.1136/adc.2009.161117.
-
Limburg H, Gilbert C, Hon do N, Dung NC, Hoang Th: Prevalence and causes of incomprehension in children in Vietnam. Ophthalmology. 2012, 119: 355-361. 10.1016/j.ophtha.2011.07.037.
-
Zepeda-Romero LC, Barrera-de-Leon JC, Camacho-Choza C, Gonzalez Bernal C, Camarena-Garcia Eastward, Diaz-Alatorre C, Gutierrez-Padilla JA, Gilbert C: Retinopathy of prematurity as a major cause of severe visual harm and blindness in children in schools for the blind in Guadalajara city, Mexico. Br J Ophthalmol. 2011, 95: 1502-1505. x.1136/bjophthalmol-2011-300015.
-
Born Too Soon: The Global Activeness Report on Preterm Nascence. Edited by: Howson CP, Kinney MV, Lawn JE. 2012, March of Dimes, PMNCH, Save the Children, World Health Organization. New York, [http://www.who.int/pmnch/media/news/2012/preterm_birth_report/en/index1.html]
-
Keeping promises, measuring results: Commission on Information and Accountability for Women'southward and Children's Health.
-
Blencowe H, Cousens S, Chou D, Oestergaard MZ, Say Fifty, Moller A, Kinney M, Lawn J: Chapter 2: 15 one thousand thousand preterm births: Priorities for action based on national, regional and global estimates. Born Too Soon: the Global Activeness Report on Preterm Birth. Edited past: Howson CP KM, Backyard JE. 2012, New York 2012: March of Dimes, PMNCH, Relieve the Children, World Health Organisation, New York, [http://world wide web.who.int/pmnch/media/news/2012/borntoosoon_chapter2.pdf]
-
O'Connor AR, Wilson CM, Fielder AR: Ophthalmological bug associated with preterm nascence. Eye (Lond). 2007, 21: 1254-1260. x.1038/sj.eye.6702838.
-
Marlow Northward, Wolke D, Bracewell MA, Samara Grand: Neurologic and developmental disability at vi years of historic period after extremely preterm birth. Northward Engl J Med. 2005, 352: nine-xix. 10.1056/NEJMoa041367.
-
Doyle LW, Ford Yard, Davis N: Health and hospitalistions later on discharge in extremely low birth weight infants. Semin Neonatol. 2003, eight: 137-145. 10.1016/S1084-2756(02)00221-X.
-
Greenough A: Long term respiratory outcomes of very premature birth (<32 weeks). Semin Fetal Neonatal Med. 2012, 17: 73-76. x.1016/j.siny.2012.01.009.
-
Mwaniki MK, Atieno 1000, Backyard JE, Newton CR: Long-term neurodevelopmental outcomes after intrauterine and neonatal insults: a systematic review. Lancet. 2012, 379: 445-452. x.1016/S0140-6736(11)61577-eight.
-
Hagberg B, Hagberg G, Beckung E, Uvebrant P: Changing panorama of cognitive palsy in Sweden. VIII. Prevalence and origin in the birth year menses 1991-94. Acta Paediatr. 2001, 90: 271-277.
-
Vocalizer LT, Salvator A, Guo S, Collin M, Lilien 50, Baley J: Maternal psychological distress and parenting stress after the nascence of a very low-nativity-weight babe. JAMA. 1999, 281: 799-805. ten.1001/jama.281.ix.799.
Acknowledgements
The Born Besides Soon report was funded by March of Dimes, the Partnership for Maternal, Newborn and Child Health and Relieve the Children. We would like to thank the Born Too Soon Preterm Birth Action committee, including the Preterm Birth Technical Review Panel and all the report authors (in alphabetical order): José Belizán (chair), Hannah Blencowe, Zulfiqar Bhutta, Sohni Dean, Andres de Francisco, Christopher Howson, Mary Kinney, Marking Klebanoff, Joy Lawn, Silke Mader, Elizabeth Mason (chair), Jeffrey Murray, Pius Okong, Carmencita Padilla, Robert Pattinson, Jennifer Requejo, Craig Rubens, Andrew Serazin, Catherine Spong, Antoinette Tshefu, Rexford Widmer, Khalid Yunis, Nanbert Zhong.
The authors appreciated review and inputs from Mark Klebanoff and Khalid Yunis. Give thanks you to Megan Bruno for her administrative back up. We would also like to thank the Bill & Melinda Gates Foundation for funding the time for Boston Consulting Group.
This article has been published as role of Reproductive Health Volume 10 Supplement 1, 2013: Built-in too soon. The full contents of the supplement are bachelor online at http://www.reproductive-health-periodical.com/supplements/x/S1.
Author information
Affiliations
Consortia
the Born Too Soon Preterm Nativity Activeness Grouping (see acknowledgement for total list)
Corresponding author
Additional information
Competing interests
The author's declare that they have no disharmonize of involvement. The authors alone are responsible for the views expressed in this article and they do non necessarily represent the views, decisions or policies of the institutions with which they are affiliated.
Authors' contribution
HB, MK and JL drafted the newspaper with SC, DC, MZO, LS, ABM. All authors reviewed the last manuscript.
Electronic supplementary textile
12978_2013_232_MOESM1_ESM.doc
Additional file 1: In line with the periodical's open peer review policy, copies of the reviewer reports are included every bit boosted file ane. (DOC 46 KB)
Rights and permissions
Open Access This article is published under license to BioMed Central Ltd. This is an Open Admission commodity is distributed nether the terms of the Creative Eatables Attribution License ( https://creativecommons.org/licenses/by/2.0 ), which permits unrestricted use, distribution, and reproduction in any medium, provided the original piece of work is properly credited. The Artistic Eatables Public Domain Dedication waiver ( https://creativecommons.org/publicdomain/zero/1.0/ ) applies to the information made available in this article, unless otherwise stated.
Reprints and Permissions
About this article
Cite this article
Blencowe, H., Cousens, Due south., Chou, D. et al. Built-in Too Soon: The global epidemiology of 15 million preterm births. Reprod Health 10, S2 (2013). https://doi.org/10.1186/1742-4755-x-S1-S2
-
Published:
-
DOI : https://doi.org/10.1186/1742-4755-x-S1-S2
Keywords
- Preterm nascence
- epidemiology
- neonatal mortality
Source: https://reproductive-health-journal.biomedcentral.com/articles/10.1186/1742-4755-10-S1-S2
0 Response to "What Is the Probability That Less Than 20 Preemies Are Born Out of the 250 Babies?"
Enregistrer un commentaire